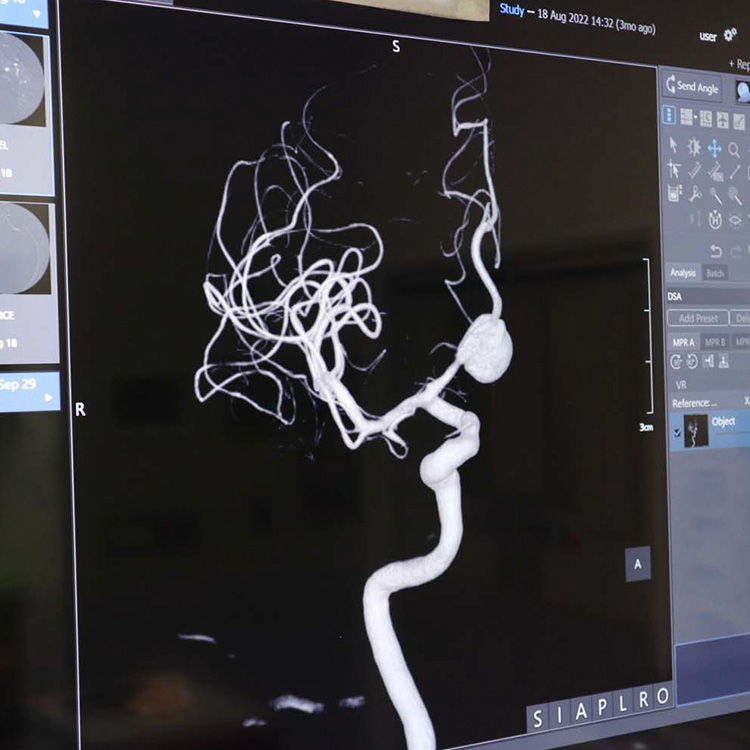
A brain aneurysm is a localised bulging of an artery in the brain due to weakness in the vessel wall. Brain aneurysms often only become symptomatic when they rupture and cause bleeding around and into the brain, known as a subarachnoid haemorrhage.
How are cerebral aneurysms treated?
There are two ways to treat cerebral aneurysms. The first involves an open surgical procedure with a craniotomy and careful dissection to expose the aneurysm, and placement of one or more metallic clips across the aneurysm neck to stop flow into the aneurysm.
The second options involves a procedure performed from within the artery itself (endovascular) and has become an alternative to surgery in many cases. By placing small, soft, platinum coils within the aneurysm via a small tube or catheter introduced from the groin, open surgery can be avoided and recovery time significantly reduced. Both treatments aims to decrease and stop blood flow from entering the aneurysm and therefore removing the risk of haemorrhage.
There are multiple factors which determine which treatment option is best for the patient. All aneurysm cases are discussed with the neurovascular interventionalist and neurosurgeon so that the best treatment option is offered.
What happens during the procedure?
Prior to the procedure your doctor will likely commence you on antiplatelet medication. It is important that you take these medications as per the instructions as these medications help to significantly decrease the risk of stroke from the procedure.
The procedure is performed in the angiography suite in Calvary Lenah Valley theatres. Here you lay on your back on a special bed with two Xray cameras.
The procedure is performed under a general anaesthetic administered by a specialist doctor called an anaesthetist.
A plastic tube is placed into the common femoral artery (the main artery to the leg) at the level of the hip joint. You are given further medication to thin your blood (through the drip) and a number of small catheters are navigated to the target location. A very small microcatheter is then advanced into the aneurysm and small platinum coils are inserted through the catheter and deployed within the aneurysm.
To ensure the coils stay in place a metal stent may need to be deployed across the neck of the aneurysm or a different stent called a flow diverting stent is deployed to further decrease flow into the aneurysm. Following satisfactory decrease in blood flow into the aneurysm or occlusion of the aneurysm all the catheters are removed. A small stitch is placed in the artery in the leg to close the hole where the small plastic catheter had been.
Once you awake from the anaesthesia you will spend a short time in the theatre recovery area and then be transferred to ICU for the night. Following the procedure you will be asked lie flat on your back for 4 hours. The day following the procedure you will generally be transferred from the ICU to a surgical ward for a further 1-2 day stay.
You must continue to take your antiplatelet medications daily until directed by the neurovascular specialist to stop. A follow up appointment will usually be booked for 1 weeks following the procedure, with a CT or MRI performed at various time intervals following the procedure.
What are the risks?
All medical procedures carry risks. Any procedure involving blood vessels of the brain is a serious procedure and there can be serious complications. However, in recommending this procedure your doctor believes the benefits of undergoing this operation exceed the potential risks involved.
Minor common complications include:
- Minor pain or bruising at the femoral artery puncture site
Minor uncommon complications include:
- infection at the arterial puncture site, allergic reactions to contrast dye, a patch of hair loss or skin reddening from a high Xray dose.
Major complications include:
- Aneurysm rupture – very rarely an aneurysm can rupture during the procedure. This can result in intracranial haemorrhage (called subarachnoid haemorrhage). A subarachnoid haemorrhage can result in severe disability or even death.
- Stroke – This occurs due to the formation of blood clots during the operation, blood vessel spasm or aneurysm rupture. This can result in severe disability including loss of movement in arms or leg, speech or swallow disturbance or visual loss. If the stroke is very large this can result in death.
- Arterial damage: damage to surrounding blood vessels (including the artery in the leg) can occur due to catheter placement.
- Retroperitoneal haemorrhage – rarely bleeding from the arterial puncture site in the leg can extend into the abdomen.
- Renal impairment – in patients who already have poor renal function the contrast dye used during the procedure can sometimes worsen renal function or even result in renal failure.
- Anaesthetic complications including issues with the lungs or heart
In a small number of cases despite treatment an aneurysm may continue to fill with blood or continue to grow. This is why it is important to monitor the aneurysm at regular intervals following the procedure. If the aneurysm fails to block off or continues to grow a subsequent procedure may be required.
When obtaining consent to perform this procedure your doctor will discuss each of these risks in detail. Please feel free to ask any questions you may have.
What are the alternatives?
There are two main options when discussing treatment of cerebral aneurysms.
The first option is to do no procedure but to perform regular CT or MRI scanning to ensure the aneurysm is stable. This option may be suitable for very small aneurysms or in people with other significant health concerns. However there is a small yearly risk that if left untreated the aneurysm could rupture spontaneously.
The second option is that an operation (either via an open surgical technique or a procedure through the artery) is performed.
All these options will be discussed with you, including the positives and negatives of each in order to come to the best and safest decision in how your aneurysm is treated.
What do I need to do after I go home?
We recommend that when you are discharged home you have a family member or friend stay for a night or two to ensure you are well and help you with jobs around the house.
We would suggest that you have at least 1-2 weeks off work following the procedure. You will also not be able to drive for two weeks following the procedure, this may be longer if the procedure is complicated by stroke or bleeding. A letter will be sent to your GP and other specialists involved in your care. This will detail what has happened to you in hospital and which medications you are on. If you have been prescribed antiplatelet blood thinners it is very important that you continue to take these until advised otherwise by your treating neurovascular doctor.
Will I have a follow-up appointment?
We will arrange a follow up appointment usually 1 week after the procedure. During this consultation Dr Bell will check for any potential complication, review your medications and discuss the plan for future imaging and follow up.